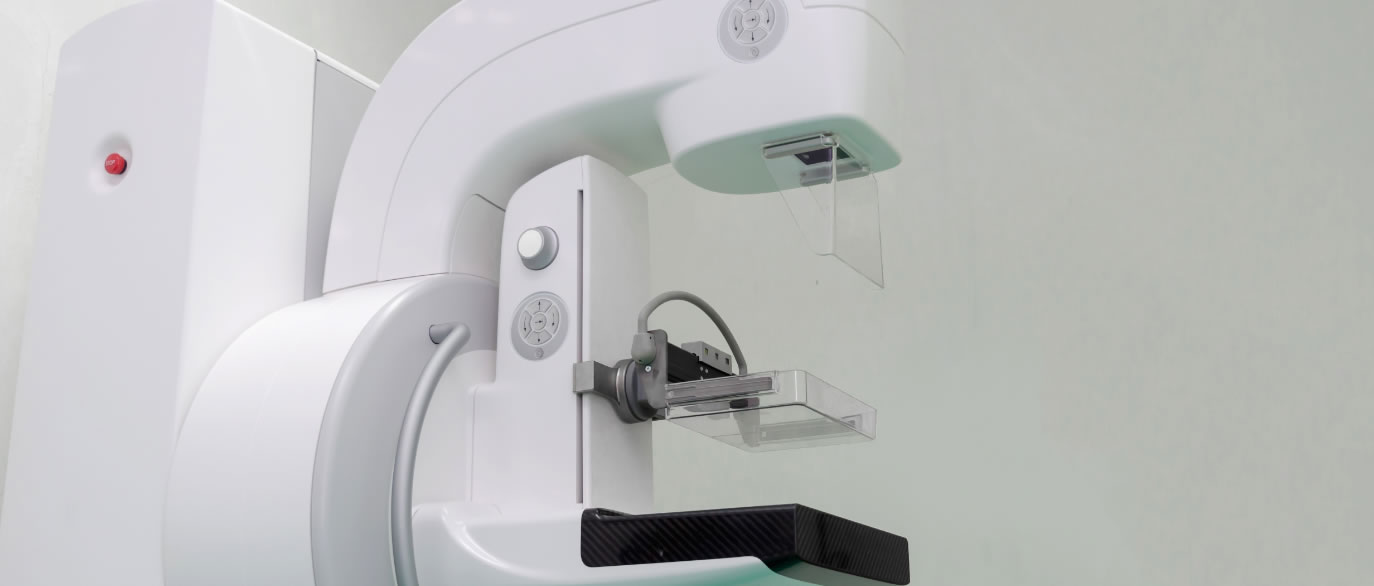
By offering state-of-the-art mammography services, MIF can provide early detection, a vital advantage in the battle against breast cancer.
The survival rate of breast cancer directly correlates with the size of cancer — the smaller the tumor, the greater the chance of survival. This is where Medical Imaging of Fredericksburg plays a crucial role in women's health.
What is a Mammogram?
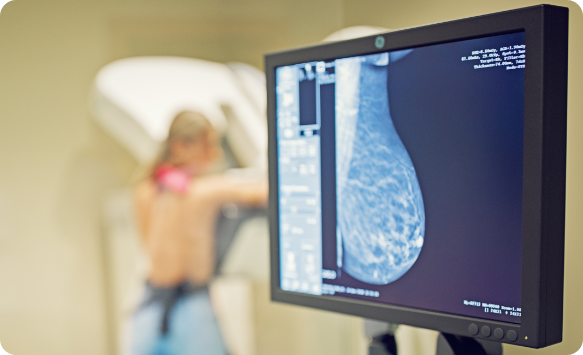
A mammogram is a low-dose X-Ray of the breasts. Mammograms can detect breast cancer up to three years before a tumor can be felt during a breast exam. Without a cure for breast cancer, early detection is the very best defense.
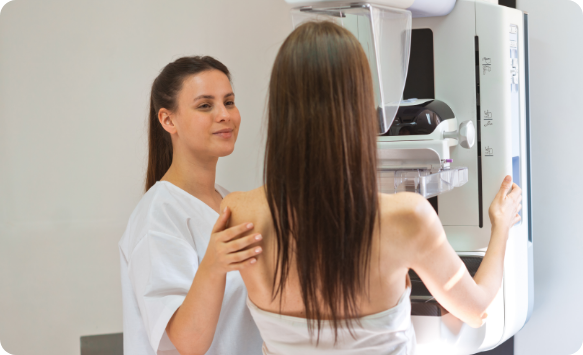
What Can I Expect?
After removing clothing from the waist up, you will stand in front of a mammography machine. The breast will then be positioned on a clear plastic plate for X-Rays on the top and bottom, as well as the sides. While the plates flatten the breast in the optimal position for the X-Ray, you will feel pressure. These steps will be repeated for both breasts. The entire process will be completed in about 15 minutes.
How Can I Prepare?
It is not recommended to schedule a mammogram the week before or during your period
Do not wear deodorant, perfume, or powder above your waist on the day of your mammogram
Wear two-piece garments such as a top and pants or a skirt, rather than a dress